Should sleeve and bypass procedures still be performed?
Dr. Le Goff - Obesity surgeon in Paris
Dr Le Goff chirurgien bariatrique
Should sleeve and bypass procedures still be performed?
The Le Goff Technique is revolutionising obesity surgery with a reversible gastroplasty method with zero mortality
Paris, 26 June 2015 – A new reversible, adjustable and non-invasive treatment for morbid obesity, the Le Goff Technique, from the name of the surgeon, Jean-Yves Le Goff who developed it, has been shown to be remarkably effective over a period of 20 years, with significant weight loss and above all, zero operative mortality, unlike other procedures currently performed.
The “Le Goff Technique” consists of a gastric banding with fixing of the band and partial gastric plicature, associated with strong psychological care. It has allowed the morbidly obese to lose on average 62% of their excess weight in five years, and as much as 70% to 100% over a period of 7 to 19 years.
“This method offers longer lasting results than simply placing a band without fixing it, with zero mortality and morbidity far lower than for the sleeve and bypass procedure”, explains Dr Jean-Yves Le Goff, at the Trocadéro Clinic and Seine-Saint-Denis private hospital.
The results of this study conducted by Dr Jean-Yves Le Goff in 794 patients assessed between 1996 and 2017 were presented at the annual Congress of the French Society for Obesity Surgery and Metabolic Diseases (SOFFCOMM) which took place in Lyon from 28 to 30 May and at the World Congress for Obesity Surgery (IFSO), in Montreal. They are published in the June issue of the review Obésité.
The purpose of the study was to compare the results of gastric banding with plicature to those of the sleeve and bypass techniques in terms of weight loss, morbidity and mortality.
Mortality, complications and weight gain
In 2014, 45,500 obesity operations were performed in France; a figure that is growing constantly. However, every year, these operations are shown to be ineffective in the medium to long-term (40 to 50 % of patients regain weight), or lead to a number of post-operative deaths in the first 30 days (113 deaths in 2011) and very high complications and repeat surgery.
Three techniques are used in bariatric surgery to treat morbid obesity: gastric banding with placing of a band, the sleeve and the gastric bypass (or mini bypass). While this method presents low post-operative mortality (4 deaths in the 30 days following the operation, PMSI data, 2011), it usually fails due to unstable fixing of the band.
The other two methods lead to high mortality: 55 post-operative deaths for sleeve surgery and 54 deaths for bypass surgery (PMSI data, 2011), high morbidity (complications) and a very high number of successive repeat operations (up to 6 to 7 times), either due to complications or due to excessive weight gain.
Certain advantages, zero mortality
The Le Goff Technique consists of gastric band surgery with partial plication of the stomach. In addition to the placing of the band, the top of the stomach is folded over (greater tuberosity) to cover the band itself. The band is attached using sero-gastric muscular-oesophageal sutures, reducing the size of the underlying stomach cavity. Gastric evacuation is slowed. This lower valve stimulates the IGLE satiety centres in the wall of the abdominal oesophagus, thus reducing appetite.
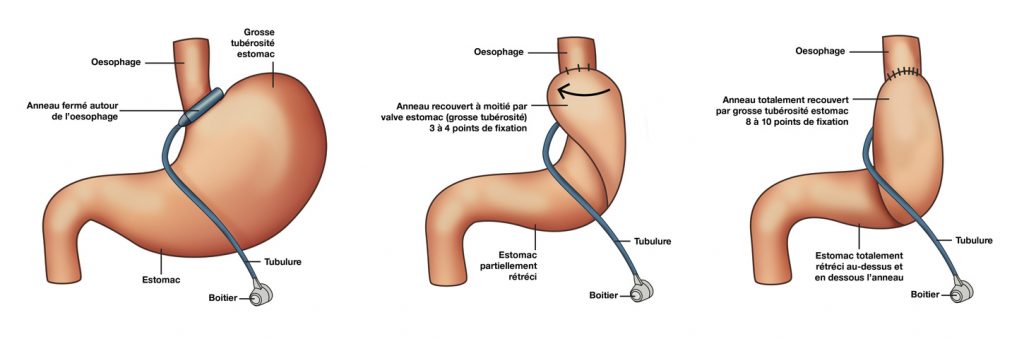
This procedure must be associated with multidisciplinary medical-surgical, nutritional, psychiatric-psychoanalytical treatment, two to four visits in the first year, with the accent firmly on the psychological factors (psychotherapy support often indicated) and a resumption of sport.
“In 1994-1995, my Belgian friend Guy-Bernard Cadière, inventor of the laparoscopic band, told me that the main issue with the band was the fact that it often slipped. A solution therefore had to be found to attach it firmly. I had the idea of folding over the upper part of the stomach on the band to be able to avail of stable anchoring points and thus reduce the stomach cavity. The problems of dilatation due to slipping are greatly reduced. Patients usually have a great feeling of satiety, with low food intake”, explains Dr Le Goff.
“This is a minimally-invasive, reversible and non-aggressive procedure without mutilations. For 19 years, it has been widely proven. This is why I am making it known today. It is an alternative to be offered without the morbidity and mortality of other types of surgery”, he adds.
This method has a certain number of advantages over the two current methods:
- Zero mortality, very low post-operative morbidity
- Reversible, adjustable, minimally-invasive procedure, without mutilations
- Very significant reduction in dilatation issues associated with ring slippage and complications
- Considerable short-, medium- and long-term weight loss with very high satiety
- No nutritional deficiencies and much higher quality of life
- Regular monitoring and treatment of patients over time
- Extremely low rate of repeat surgery
The importance of psychological care
This surgical procedure is part of a multidisciplinary treatment, in particular with visits to the psychiatrist-psychoanalyst and the nutritionist.
“These pre-surgical consultations promote the patient’s engagement with the gastric band project. Often it underlines the importance of psychological factors at the origin of morbid obesity, present in 80 to 90 % of cases, and helps patients to understand why this monitoring is essential and vital in successfully losing weight, to recover one’s physical and mental health”, explains the psychiatrist Didier Pons.
About Dr Jean-Yves Le Goff
Dr Jean-Yves Le Goff is a laparoscopic digestive surgeon. Specialist in obesity surgery, he works at the Trocadéro clinic and at the Seine Saint-Denis (Le Blanc-Mesnil) private hospital. Formerly assistant clinical manager and resident in Paris hospitals, he is the founder and former manager of the endoscopic surgery unit at Bichat Hospital (1988-97). He is also a founding member of the French Society for Endoscopic Surgery (SFCE), the European Association for Endoscopic Surgery (EAES) and the Foundation for the Development of Laparoscopic Surgery (FDCL). He is also a member of the French Society for Obesity Surgery (SOFCO).